One year ago, Marie, 32, was homeless, addicted to fentanyl, and living off whatever money her family and friends would send. She spent many nights with her boyfriend in his muscle car, parked along Mount Tabor, shivering to avoid using valuable gas in the tank for heat. Other nights, she squatted in a vacant apartment on Southeast Powell Boulevard.
One morning last summer, she woke up feeling nauseous.
She was pregnant.
For Marie, a Franklin High School dropout who says she smoked up to 50 fentanyl pills a day, it was another complication in an already tangled life. Her feet swelled up from sleeping upright in a car seat, and when cuts stopped healing, it was because she had developed gestational diabetes.
But it turned out her pregnancy was a ticket to housing and sobriety.
Fentanyl addiction is difficult to subdue, but it is treatable. Drugs, given to Marie while she was still in Vancouver’s PeaceHealth Southwest Medical Center following the delivery of her son, reduced the cravings. And for new mothers like Marie, there’s an added spur: the threat of the state taking their children.
“Nobody believed I could do it. Nobody had any faith in me at all,” she says. “But I wasn’t going to lose my kids.”
There was reason to doubt her. Marie already had one child, a 10-year-old daughter who goes by Tink, yet she continued using heroin daily. After the state briefly put Tink in foster care when she was a kindergartner in 2017, Marie got clean and got her daughter back, but stayed sober only a few years.
Fentanyl is so prevalent, Marie says, that she was offered the drug while smoking a cigarette in front of the Vancouver hospital where she gave birth this past May.
So, to stay off the drug that nearly destroyed her life, Marie needed to stay off the street.
It was the same need that confronts the estimated 70,000 Oregonians who battle opioid use disorder. But Marie, unlike many others, found a way out.
That haven is an eight-bedroom ranch house in Southeast Portland where Marie now lives with seven other moms, all trying to stay sober. The house was partly funded by Measure 110—the drug decriminalization measure passed in 2020 and now under intense scrutiny and facing possible rollback.
Laura Hall runs the house and three others. “We have villainized substance use disorder for so long, and now we’re finally starting to say these are real people and we’re going to treat them respectfully,” Hall says.
Oregon is seemingly overwhelmed by narcotics and convulsed in a debate about how to combat them. The arguments are often ugly: Should people addicted to fentanyl (which is now the opioid causing the most fatal overdoses) be forced into treatment by the threat of jail, or left at the mercy of their cravings? Will compelling people to seek treatment work better than the wretched status quo, or is it just a way to put miserable people where others don’t have to see them?
Marie’s story offers clues. Her journey not only illustrates the depth of the challenges Oregon faces in pulling itself out of this crisis, it also provides a road map for what successfully doing so might eventually look like.
Dr. Todd Korthuis, head of the addiction medicine section at Oregon Health & Science University, offers this important truth: Fentanyl may grip the state, but users can escape the drug’s hold.
“Treatment works,” Korthuis says. “If people can stick with it, the treatment community will stick with you.”

The squat, midcentury ranch in the Hazelwood neighborhood of Southeast Portland where Marie lives has a two-car garage, a lawn dotted with towering firs, and a plastic jack-o’-lantern on the porch.
Inside, the house has the feeling of a college dorm. The garage and upstairs have been remodeled so the 2,500-square-foot home has eight bedrooms and two kitchens. There’s a line of strollers in the garage. A 7-week-old infant murmurs to himself in an electric baby swing.
Eight moms and eight children—six of them less than a year old—live in this house. All the moms are recovering from addiction.
There are an estimated 3,000 beds in sober homes like this one across Oregon. Most require the tenants to pay their own rent, although that’s increasingly being covered by insurance and grants.
Some houses are self-run, forming a community of like-minded people in recovery.
Others offer “wrap-around” services, which include a live-in peer mentor, rides to the methadone clinic, and a caseworker on hand to help with apartment hunting. At Hall’s, the goal is to move tenants into permanent housing within six months.
“If you don’t have housing that’s conducive to your recovery, it’s incredibly hard to stay sober,” Hall says. “It’s the most important thing.”
The rules of the house where Marie lives are simple. Go to meetings and treatment, get back by curfew, and don’t use drugs.
Having mothers and infants in such close proximity can create tensions. Inevitably, while one mom is desperately trying to get her infant to nap, another child is crying. There’s the occasional dispute over whose food in the refrigerator is whose—recently, Eggos began mysteriously disappearing from the freezer.
The advantages of communal living, particularly when you’re trying to parent and fight a disease at the same time, are numerous. The moms carpool to the store, cook house dinners, and take each other’s kids on walks to the park. They swap parenting advice and baby clothes.
And they know their housemates share a similar demon. “It’s nice to have people who relate to it, and don’t feel bad about it,” one of the women explains.
For many, the hardest part was getting here.
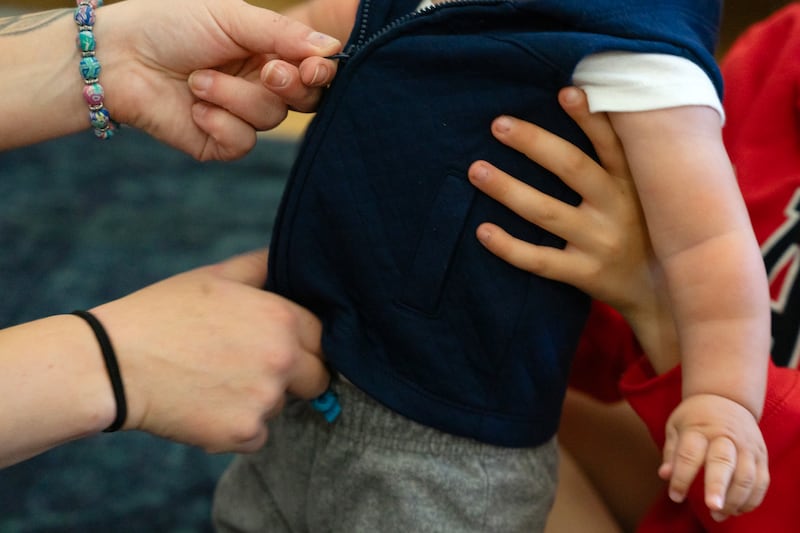
This past March, Marie was seven months pregnant and desperate. She found a ride up Marquam Hill in the pouring rain to OHSU, smoked her last two fentanyl pills at a nearby bus stop, and walked into the emergency room.
Marie had nowhere else to turn. A high school dropout whose parents were addicted to meth and opioids, she was raised by her grandmother and struggled with substance abuse for her entire adult life. (WW is using the middle names of some women in this story to protect their privacy.)
But when her grandmother died in 2021, she lost the one person she could count on.
After the landlord changed the locks on her grandmother’s apartment, Marie sent Tink, then 8, to live with her estranged mother while Marie went to the streets—and to fentanyl. That’s where she found out she was going to have another child, and spent much of the pregnancy sleeping in her boyfriend’s car.
When she walked into the OHSU emergency room, she unwittingly entered Project Nurture, a little-known program operated by local hospitals. It shuttles mothers addicted to drugs from hospital emergency rooms and maternity centers into treatment and housing.
“She was sick. We got her medicine, we got her a safe place to heal—and she got better,” says her doctor, Kea Parker.
That might sound simple, but treating fentanyl addiction is anything but.
Marie walked out of OHSU with a prescription for Suboxone, which reduces opioid cravings and has become a leading treatment for heroin addiction since being approved by the Food and Drug Administration two decades ago.
Fentanyl, a drug up to 50 times more potent than heroin, has proven to be a different beast. “It’s like crack to cocaine,” says Tony Vezina, who chairs the state’s Alcohol and Drug Policy Commission and runs a Portland-area youth recovery center. “It changed the game. We don’t know how to fully deal with it yet.”
In practice, that means the process of “detoxing” off the drug can take weeks instead of days. Due to its strength and chemical makeup, fentanyl stays in the body longer, which can cause serious withdrawal symptoms even after a patient has begun Suboxone.
Although the drug has helped many users kick fentanyl, it didn’t work for Marie. She started taking it while pregnant, but the feeling of intense anxiety that could only be relieved by fentanyl did not go away, and she soon went back to the blue pills.
She’d go back to the clinic, say whatever needed to be said to refill the prescription, then traded it for fentanyl on the street—where it, like every drug, has a price. “Left to my own devices, I was just telling them whatever to get as many Suboxone as I could get to sell,” Marie says. “I was high. It was not rational thinking.”
But, in April, when she went into labor at a hospital in Vancouver, she was put on a different drug: methadone.
Methadone is a synthetic opioid that, properly used, can reduce the cravings for illicit, more dangerous opioids. Unlike Suboxone, which only partially activates the brain’s opioid receptors and is less likely to lead to an overdose, methadone is a Schedule II drug and federal regulations require patients to go to clinics routinely to dose. In the hospital, doctors quickly ramped up her dosage and Marie’s cravings were all but eliminated, she says.
“I wish we had the systems in place where we could do that for everyone,” says OHSU’s Parker.
But getting clean is one thing. Staying clean is another.
In May, Marie moved into the Hazelwood ranch home the same day she stepped out of the Vancouver ICU with her newborn son. She was reunited with her daughter Tink the same night.
She now had a powerful ally in her fight to stay sober, a 47-year-old woman named Laura Hall.
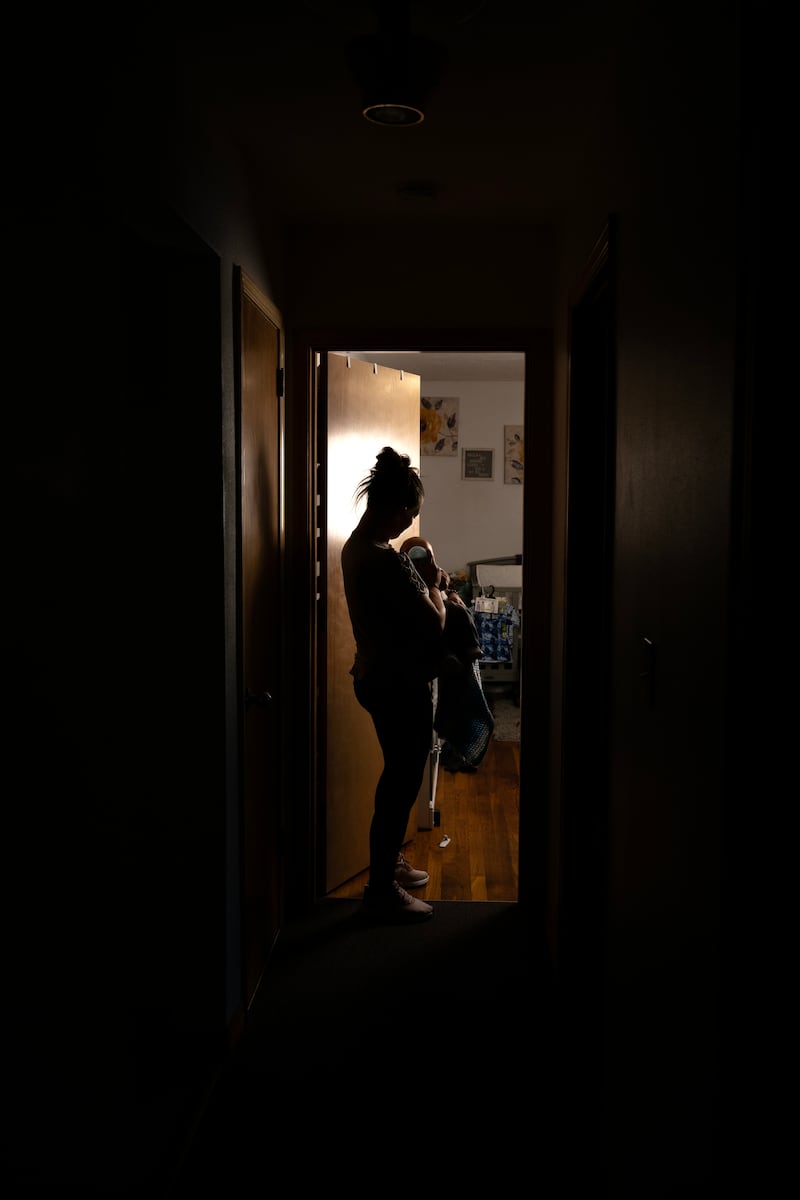
Hall is 17 years sober herself from alcohol and other drugs. She’s spent her life helping other women achieve the same, first as an advocate at the Rose Haven community center for homeless women, and then, for nearly a decade, as a caseworker for the state’s child welfare division.
Hall isn’t the sort of person who can turn down someone in need. In one recent case, her husband says, she was late for a party because she’d stopped to offer a sweater and wait for an ambulance for a naked woman outside a Taco Bell.
Her lifelong dream has been to open an apartment complex for mothers in recovery.
The state badly needs more recovery housing. Researchers at the OHSU-PSU School of Public Health recently found that Oregon has only half the number of beds it needs.
In 2021, when Hall registered a new nonprofit called Project Patchwork with the IRS, it seemed impossible. “If I win the lottery, that’s what I thought I’d do with the money,” Hall says. “It was a total pipe dream.”
Project Patchwork had only $6,500 to its name in 2021, thanks to a donation from a family member and the sale of her husband’s truck.
Then she hit the jackpot. In 2020, Oregon voters passed Measure 110, which decriminalized small amounts of hard drugs and funneled the proceeds of cannabis taxes into a new grant program to fund treatment services (see “Corrective Measures”).
The next winter, in 2021, Hall asked the state for $550,000.
Measure 110 directed the Oregon Health Authority to fund a variety of services, from harm reduction to addiction treatment to housing. But when the agency realized it had extra cash, it sought out housing providers, like Hall. “The universe is telling me to do this,” she thought.
Related story: Does the treatment promised by Measure 110 need more teeth?
Hall had planned to lease apartments, but with the promised new cash, a total of $1.1 million, her ambitions grew. When she opened her Milwaukie post office box to find the first payment, a $450,000 check, she quit her state job and started house hunting.
In December, she purchased a five-bedroom house on a quiet street in North Portland, for around $650,000. She ordered furniture from Amazon and mattresses from IKEA, and solicited donations. A stranger dropped off a load of nightstands.
Two weeks after closing on the house, the first tenant moved in: a woman in her mid-40s in recovery from meth addiction who’d set fire to her previous apartment.
Less than a year after cashing that first check, Hall now operates four homes—23 beds in total. She opened the eight-bedroom ranch in Hazelwood in May (it’s a rental). She will soon have received nearly $900,000 in total from the state.
“I didn’t want to sit on the money when I knew people were suffering,” she says.
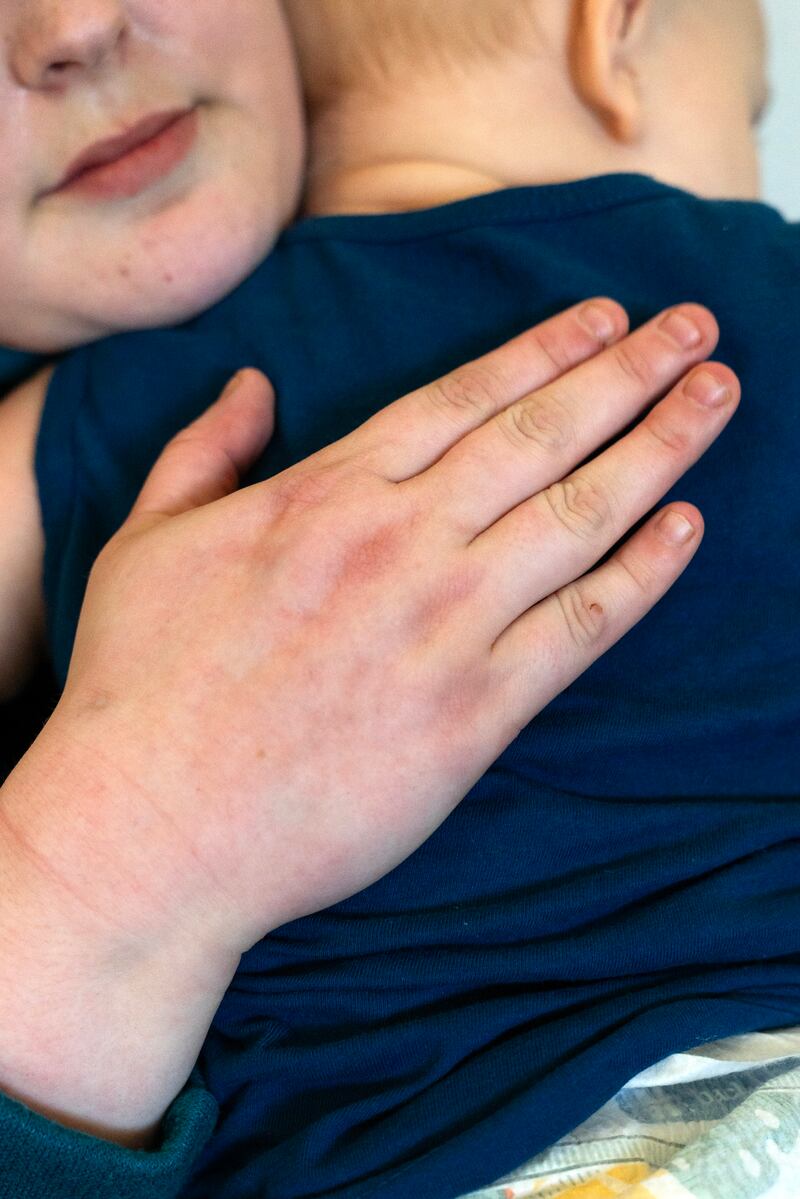
Among Hall’s new tenants is Lynn, 25, who took a room in the basement.
Lynn had arrived in Oregon a few years earlier from a one-stoplight town in North Carolina. She says she was sexually abused as early as age 11. In high school, she began using heroin—and meth, which her mom cooked.
She and a boyfriend had a child together, but lost custody of the baby two years later. “We want to break the cycle,” the caseworker told her as she took the kid away. Lynn hasn’t seen her son since, although she hunts for photos of him posted by his adopted mother on Facebook.
After accumulating a string of arrest warrants, she fled with her boyfriend four years ago—first to Tillamook, then to Portland, where they parked near Southeast 122nd Avenue and Division Street. There, she was introduced to “blues,” Portland’s slang for the counterfeit fentanyl pills popular at the time on the streets. “It was a whole other ballgame,” she says. “Waking up and having to have it.”
Then, she became pregnant.
Lynn promised herself she would do anything possible not to lose another kid. “I can’t go through the pain of not being able to do it again,” she says, “to push out a baby and say goodbye?”
When Lynn’s caseworker first met her, she wasn’t optimistic. Lynn told her she was a heavy user with a history of incredible trauma.
Indeed, for a while, Lynn would detox, go through some residential treatment, and then head immediately back to the street and relapse, all while pregnant.
In moments of doubt, her caseworker, Healtherlin Rummel, would reassure her: “You’re battling an addiction. And sometimes the addiction is greater than the love we have for our children.”
Lynn says she wasn’t chasing a high. Fentanyl no longer provided that relief. Instead, using it was almost instinctual, a habit formed from more than a decade of use. “This is all I’ve known since I was 12 years old,” she says. “If somebody has drugs around me and they offer it to me, I’m doing it before I even realize I’m doing it.”
Earlier this summer, still struggling to stay clean while caring for a toddler, Lynn called a number on a rehab bulletin board. It was Hall’s, with an offer of someplace safe to stay.
Unlike the other places Lynn had stayed, Hall’s house felt like home. She met Marie, who also knew what it was like sleeping on the streets while pregnant.
When Lynn’s son got sick, Marie offered some of her baby Tylenol. They became best friends. “It’s more than a friendship,” Lynn says. “It’s somebody who understands what I’ve been through,” Marie explains.
Lynn is six months clean, the longest streak she can remember since spending eight months in a North Carolina jail. She credits Hall. “Laura’s given me a chance,” she says. “I never thought in a million years I’d come this far.”

The typical stay at the house is four to six months, and the time Marie and Lynn will spend in Hazelwood is ticking down. Lynn is apartment hunting, making her way through a packet of 25 applications.
Marie has already found one, a subsidized apartment in Happy Valley. She plans to move in next month.
On a recent bright Saturday morning, she and Laura Hall were sitting in the shade overlooking a green field in the Southwest Portland hills—two soccer moms who seemed no different from the other parents gazing with pride at their uniformed kids.
Hall runs her two kids’ Milwaukie’s youth soccer league, and her husband coaches one of the teams. After learning Tink was the same age as her daughter, Hall signed her up for the league.
Tink has taken to the sport with the enthusiasm that only a 10-year-old girl can muster. She’d slept in her maroon soccer kit—jersey, shorts and all—Marie reported with a laugh.
Marie rolled her 4-month-old son in his stroller over to the sidelines, where someone offered her a spot in the shade under their canopy. The ball rolled out of bounds, and Tink beelined from the field, midplay, to give her brother a kiss.
The final whistle blew. Tink’s team lost—it was a rout, actually—but Tink seemed like she couldn’t care less. She was panting and smiling. Her team’s used to being the underdogs, Hall says.
Sitting in the car, later, Marie put down her phone and took in the moment, a meditative practice she’s been working on recently. When Marie’s grandmother died, she says she never thought she’d ever be happy again.
And yet, here she is now: so happy, so full of hope. “This is so cool,” she says. “I cannot believe it.”

